Work Hours
Monday to Friday: 7AM - 7PM
Weekend: 9AM - 12PM
Pressure Sores: What Every Carer, Patient and Clinician in Ireland Needs to Know
*Written by Eimear O’Rielly-(Hospital OT) at the request for Disability Ireland
As an occupational therapist, one of the things I find myself saying most often is this: pressure sores are almost always preventable. Almost. And yet, across hospitals, nursing homes and home care settings in Ireland and Northern Ireland, they remain one of the most common — and most distressing — complications for people with limited mobility.
Whether you’re a carer supporting a family member at home, a nurse or OT working in a clinical setting, or someone who has recently been told they’re at risk, this guide will walk you through what pressure sores are, why they happen, and most importantly, what can be done to prevent them.
What Is a Pressure Sore?
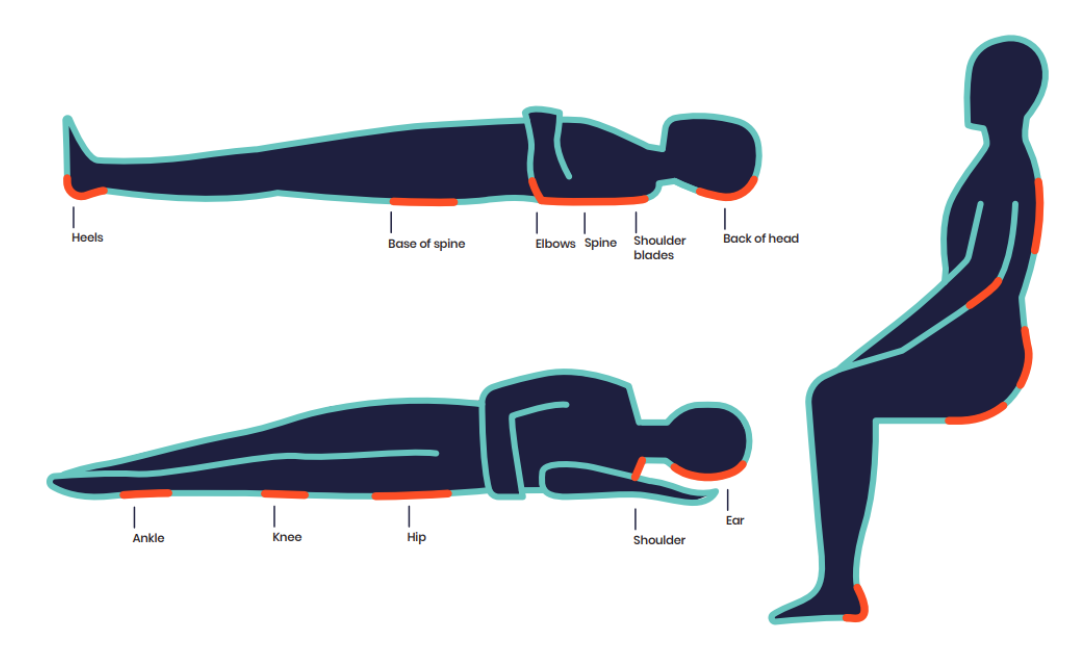
A pressure sore — also called a pressure ulcer, bedsore, or decubitus ulcer — is an area of damaged skin and tissue caused by prolonged pressure, usually over a bony prominence. The most common sites are the heels, sacrum (base of the spine), hips, elbows, and the back of the head.
Pressure sores are graded from Category 1 (non-blanching redness of intact skin) through to Category 4 (full-thickness tissue loss exposing bone, tendon or muscle). Category 3 and 4 ulcers can take months or even years to heal, carry a serious risk of infection, and in vulnerable individuals can be life-threatening.
The HSE clinical guidelines on pressure ulcer prevention are clear: prevention is always preferable to treatment. A Category 4 wound that could have been avoided with a proper pressure-relieving cushion or mattress represents not just significant patient suffering, but enormous cost to the health system.
Who Is Most at Risk?
In my clinical experience, the patients at highest risk tend to share a combination of the following factors:
- Limited or no ability to reposition themselves independently
- Reduced sensation — particularly relevant in spinal cord injury, stroke, and diabetic neuropathy
- Incontinence — moisture significantly increases skin fragility
- Poor nutritional status — skin integrity depends heavily on adequate protein and hydration
- Cognitive impairment — those with dementia may not communicate discomfort or reposition themselves
- Recent surgery — particularly prolonged procedures where patients are immobile on an operating table
Formal risk assessment using a validated tool such as the Waterlow Scale or Braden Scale should be completed on admission to any care setting, and reviewed regularly. In community settings, this is typically the responsibility of the public health nurse or community OT — but family carers play a vital role too.
The Role of Pressure Relief Equipment
Equipment alone won’t prevent pressure sores — repositioning, nutrition, skin care and clinical oversight all matter enormously. But the right equipment makes an enormous difference, particularly for those who cannot reposition themselves independently.
Pressure Relief Cushions
For wheelchair users and those who spend significant time seated, a good pressure relief cushion is one of the most important interventions available. Standard foam cushions — including most standard wheelchair cushions — provide minimal pressure redistribution and should not be considered adequate for at-risk individuals.
Clinically appropriate options include:
- Gel cushions — distribute pressure evenly and are well tolerated by most patients. Suitable for moderate risk.
- Alternating air cushions — cyclically inflate and deflate to vary pressure points. More appropriate for higher risk individuals.
- Foam contour cushions — shaped to the body to redistribute pressure away from bony prominences. Good for home use.
The Disabled Living Foundation (DLF) publishes independent guidance on selecting pressure cushions, which I regularly recommend to patients and carers in both the Republic and Northern Ireland.
Pressure Sore Pads and Protective Dressings
For patients who already have a Category 1 or early Category 2 pressure sore, or who have identified high-risk skin areas, pressure sore pads and protective foam dressings can provide a layer of localised protection while the underlying repositioning and care plan is implemented.
These are particularly useful over heels and elbows — areas that are difficult to fully offload with standard cushions or mattresses. They are not a substitute for proper pressure relief but serve as a useful adjunct, especially in the early stages of concern.
It’s important to note that wound management once a sore has broken down should always involve a tissue viability nurse or wound care specialist. Self-managing a Category 2 or above wound without clinical input is not advisable.
Practical Prevention: What Carers Can Do
If you’re caring for someone at home who is at risk of pressure sores, here is what makes the biggest practical difference:
- Reposition every 2 hours for bed-bound patients — use a repositioning chart to keep track
- Check the skin daily — particularly heels, sacrum and hips. Early redness that doesn’t fade when pressed needs attention immediately
- Keep skin clean and dry — use barrier creams in cases of incontinence
- Encourage fluid and protein intake — skin heals and resists damage far better when the person is well nourished
- Invest in appropriate equipment — a proper pressure relief cushion for the chair and an appropriate mattress for the bed
- Ask for a community OT assessment — your GP can refer, and it’s free through the HSE. An OT can assess the full picture and recommend specific equipment
Getting Equipment in Ireland and Northern Ireland
In the Republic of Ireland, some pressure relief equipment may be available on loan through the HSE Community Equipment Service. This service varies by region, so it’s worth contacting your local HSE community care team directly.
In Northern Ireland, equipment may be available through the relevant Health and Social Care Trust. Contact your district nurse or community OT for a referral to the community equipment service in your area.
For those who need to purchase equipment privately — whether because of waiting lists, specific clinical needs, or personal preference — Disability Ireland stocks a range of pressure relief cushions and pressure sore pads suitable for home use across Ireland and Northern Ireland. If you’re unsure what’s appropriate for your situation, we’re happy to help guide you — just get in touch.
When to Seek Clinical Help Immediately
Please don’t wait if you notice any of the following:
- Skin that is persistently red and doesn’t return to normal colour within 30 minutes of pressure being relieved
- Any open wound, blister, or broken skin over a pressure area
- Skin that looks or feels different — hardened, boggy, or discoloured
- Signs of infection — increased warmth, swelling, discharge, or odour from a wound
Contact your GP, public health nurse, or district nurse immediately in these cases. In more urgent situations, your local injury unit or emergency department can assess and treat pressure wounds.
A Note From Disability Ireland
We know that navigating pressure sore prevention can feel overwhelming — especially if you’re a carer doing your best for someone you love, or a clinician looking for reliable suppliers. We stock a carefully selected range of pressure relief cushions and pressure sore pads suitable for home and clinical use, and we serve customers across the Republic of Ireland and Northern Ireland.
If you have questions about which product is right for a specific situation, please don’t hesitate to get in touch. We’re not here to just sell you something — we’re here to help you find the right solution.